
Services
In recent years, we’ve made important strides in our efforts to advance quaternary services. We offer treatments that are not readily available elsewhere in the region, and we have invested in the people, systems and technology that help us set the pace in cardiovascular innovation and care.
Cardiovascular Diagnostic Imaging: 612-775-4200612-775-4200
Mobile Diagnostics: 612-775-4222612-775-4222
Allina Health Minneapolis Heart Institute is a recognized leader in raising the standard of care for advanced cardiovascular imaging. Our imaging specialists have:
- Helped develop appropriateness guidelines for cardiac computed tomography angiography (CCTA) and cardiac magnetic resonance imaging (MRI).
- Worked with the Intersocietal Commission to develop cardiac CT board examination and the CT lab accreditation criteria.
- Led cardiovascular CT education through leadership in the Society for Cardiac Computed Tomography.
Center for Advanced Cardiovascular Imaging
Our program offers patients comprehensive cardiovascular imaging services, including dedicated adult and pediatric cardiovascular CT and MRI. Our patients have seamless access to tests and treatment in one convenient location, often on the same day if needed.
In addition to comprehensive services at Abbott Northwestern Hospital in Minneapolis, our mobile echo and vascular imaging technologies bring these services to patients in their communities at our conveniently-located outreach sites.
Advanced imaging capabilities allow our subspecialty experts to develop unique treatment approaches for vascular disease, genetic arrhythmias and heart failure. Cardiologists and radiologists from around the world come to Allina Health Minneapolis Heart Institute for specialized training.
The Allina Health Minneapolis Heart Institute echo lab accomplishments include:
- Transesophageal echocardiography (TEE) and 3D echo support for the Valve Center
- Strain Imaging: a new non-invasive method for assessment of myocardial function
- TEE support of complex surgical procedures
- TEE cardioversions: a new process with one-time anesthesia for patients undergoing cardioversion and TEE
For the growing number of patients with advanced heart failure, successful outcomes depend on consistent, evidence-based clinical management and expert heart failure practitioners. The highly skilled multidisciplinary team at the Center for Advanced Heart Failure Treatment delivers comprehensive care for the most complex, endstage heart failure patients. They offer the full spectrum of therapeutic options, from traditional treatment to breakthrough approaches on the forefront of technology.
Allina Health Minneapolis Heart Institute physicians are in close communication with partnering physicians throughout the patient’s care—from diagnosis of early heart failure through advanced treatment. They are available 24/7 to discuss any heart failure concerns.
The team includes:
- Specialized cardiologists who are board certified in Advanced Heart Failure Therapies and Transplant
- Cardiac surgeons
- Doctors of pharmacy
- Certified nurse practitioners and physician assistants
- Nurses, including specialized care coordinators
- Dietitians
- Social workers
- Exercise physiologists
- Support staff
Immediate Transfer of Patients In Cardiogenic Shock
Patients in cardiogenic shock who require advanced mechanical support benefit from the rapid response and transfer protocols that are supported by the Allina Health Minneapolis Heart Institute’s established network of partner community hospitals and its highly skilled and experienced clinical team.
Heart Transplantation
When tailored medical therapy is not enough, heart transplantation may offer a life-saving treatment option for patients with end-stage heart failure. Since establishing a new team and reorganizing the program in 2010, 38 transplant procedures have been performed at Allina Health Minneapolis Heart Institute – Minneapolis (as of June 2012). Abbott Northwestern’s Heart Transplant Program is Centers for Medicare & Medicaid Services certified.
Ventricular Assist Devices (VADs)
A variety of temporary and long-term mechanical circulatory support devices are available, specific to each patient’s need. These devices are an important option as a bridge to cardiovascular recovery, a bridge to transplantation or as a destination therapy for permanent support. The VAD Program received Joint Commission Certification for VAD Destination Therapy in November 2010.
Cardio-oncology
Our cardio-oncology program evaluates and treats the cardio-toxic side effects of chemotherapeutic agents and identifies patients at risk for future adverse events. Working closely with oncologists, the goal of the cardio-oncology team is to help patients complete their treatment, giving them the best possible chance for a cure.
Pioneering Research
With the support of the Minneapolis Heart Institute Foundation, advanced heart failure specialists are involved in FDA-approved and National Institutes of Health (NIH)-sponsored trials for:
- Novel heart failure therapies
- New generation VADs
- Adult stem cell angiogenesis
Cardiac surgery at Allina Health Minneapolis Heart Institute has always maintained an exceptionally high level of quality and expertise. With increased emphasis on system-wide program development, cardiac surgeons are advancing innovative surgical therapies and creating new options for patients. A true multidisciplinary focus allows surgeons and cardiologists to collaborate with patients to develop optimal individualized treatment plans.
Allina Health Minneapolis Heart Institute cardiac surgeons have nearly 100 years of combined experience, offering expertise and options that are not available at most other hospitals in the region. They perform a range of complex procedures including:
Complex Structural Heart Surgery
- Ventricular assist devices for end-stage heart failure and total artificial heart surgery
- Heart transplants
- Transcatheter valve procedures in partnership with interventional cardiologists
- Adult congenital heart surgery in partnership with pediatric cardiac surgeons
- Valve-sparing root, complex mitral valve (including bi-leaflet repairs) and tricuspid valve repairs
Surgery for Arrhythmias
- Concomitant atrial fibrillation surgery
- Lone atrial fibrillation surgery
Surgery of the Great Vessels
- Complex aortic aneurysm surgery including the transverse arch
- Aortic dissection surgery
High-risk Coronary Artery Bypass
Less Invasive Approaches to Conventional Surgery
Research
Ongoing clinical investigation sustains the leadership role of academic institutions. Surgeons at Allina Health Minneapolis Heart Institute are participating in more than 25 ongoing clinical research trials. Every year, they publish many peer-reviewed manuscripts and are frequent presenters of abstracts at national and international meetings. Our surgeons are also invited lecturers nationally and internationally.
Resources
- Patient education open heart surgery videos. Patient videos include: What to expect, breathing exercises and tips for getting up and down.
- HeartValveSurgery.com
Allina Health Minneapolis Heart Institute created the first comprehensive cardiovascular emergency center capable of immediately triaging and treating all forms of cardiovascular emergencies, not just acute myocardial infarctions or heart attacks. Modeled after Level One trauma programs and based on Allina Health Minneapolis Heart Institute’s first-in-the-nation ST-segment elevation myocardial infarction (STEMI) transfer program, the Cardiovascular Emergency Center is ready for any cardiovascular emergency including cardiac arrest, ascending aortic dissection, abdominal aortic aneurysm (AAA), critical limb ischemia, STEMI, non-STEMI/unstable angina and cardiogenic shock.
The Cardiovascular Emergency Center is made possible because of the depth and breadth of services available at Allina Health Minneapolis Heart Institute and features a board-certified cardiologist inhouse 24/7. Emergency teams are always ready and provide the most advanced therapies available, such as therapeutic hypothermia and all forms of cardiovascular surgery including ventricular assist devices (VADs). Allina Health Minneapolis Heart Institute’s Cardiovascular Emergency Center is the most comprehensive program of its kind in the nation.
Level One Heart Attack Program
When a patient is diagnosed with STEMI, the goal is to open the blocked artery within 90 minutes or less, from the time the patient arrives at a community emergency department to the start of life-saving percutaneous coronary intervention (PCI) at Abbott Northwestern Hospital. This is achieved through a standardized process with statewide emergency care providers who stabilize the patient and begin adjunctive therapies even before the patient arrives in Minneapolis. When a Level One emergency is declared, all systems and personnel are set in motion, communication is frequent and thorough, and the patient is transported directly to a waiting, expert PCI team—anytime, day or night.
Therapeutic Hypothermia (Cool It)
Allina Health Minneapolis Heart Institute pioneered the collaborative “Cool It” protocol and was the first to simultaneously combine transport, emergency angioplasty and cooling. The core body temperature of a patient resuscitated after cardiac arrest is cooled to 33° C to reduce the risk of permanent neurological damage.
Aortic Dissection
In 2005, Allina Health Minneapolis Heart Institute created a multidisciplinary aortic dissection program to aid in the emergency room recognition, triage and surgical treatment of these critically ill patients. Through regular updates to the regional network partners, the time to diagnosis this condition has been cut by 43 percent (or by 4.5 hours at community hospitals) and the time to surgical treatment has been cut in half. For a condition with a 1 percent per hour mortality rate, this has dramatically improved care. On a local level, the multidisciplinary team of cardiologists, cardiac and vascular surgeons, emergency room physicians, radiologists and cardiac anesthesiologists meets regularly to review cases and treatment times to continue to improve care. Care protocols for patients with suspected and confirmed aortic dissection are available. Patients are encouraged to return to the aortic dissection clinic for regular follow-up care that includes complex imaging studies.
Critical Limb Ischemia
Peripheral arterial disease can manifest as critical limb ischemia. Prompt diagnosis and treatment are mandatory to prevent limb loss. Treatment algorithms are designed to help referring clinicians diagnose critical limb ischemia (and all other cardiovascular emergencies) and facilitate transfer. Emergent endovascular and surgical therapies are provided by the Allina Health Minneapolis Heart Institute vascular surgery team.
Ruptured Aortic Aneurysm
Allina Health Minneapolis Heart Institute vascular surgeons adapted the Level One Heart Attack protocol to ensure faster diagnosis and emergency treatment of thoracic and abdominal aortic aneurysms. As a result, time from diagnosis to intervention dropped by more than an hour. Combined with increased use of endovascular therapy, survival outcomes improved from 69 percent to 89 percent for these historically deadly vascular emergencies2.
Non-STEMI and Unstable Angina
Allina Health Minneapolis Heart Institute – Minneapolis is Minnesota’s first Accredited Chest Pain Center, as designated by the Society of Chest Pain Centers. The Chest Pain Program applies protocol-based care to reduce variations in treatment and create a more efficient and effective way to treat patients with all types of acute coronary syndromes, not just STEMI. One of the first multi-hospital initiatives for this condition nationwide, the program clearly identifies which patients need to be transferred to Abbott Northwestern and which can safely remain in their communities for testing and follow-up.
Current or past online issues of Allina Health Minneapolis Heart Institute Level One Report
- Level One Report 2018 (Published May 2019)
- Level One Report 2017 (published May 2018)
- Level One Report 2016 (published May 2017)
- Level One Report 2015 (published May 2016)
Cardiovascular Emergency Partner Hospitals
- Aitkin – Riverwood Healthcare Center
- Alexandria – Douglas County Hospital
- Arlington – Sibley Medical Center
- Blue Earth – United Hospital District
- Brainerd – St. Joseph’s Medical Center
- Cambridge – Cambridge Medical Center
- Chaska – Two Twelve Medical Center
- Crosby – Cuyuna Regional Medical Center
- Faribault – Allina Health Faribault Medical Center
- Glencoe – Glencoe Regional Health Services
- Grand Rapids – Grand Itasca Clinic and Hospital
- Grantsburg,WI – Burnett Medical Center
- Hutchinson – Hutchinson Medical Center
- LeSueur – Minnesota Valley Health Center
- Litchfield – Meeker County Memorial Hospital
- Minneapolis – Abbott Northwestern Hospital
- Monticello – New River Medical Center
- Mora – FirstLight Health System
- Morris – Stevens Community Medical Center
- New Prague – Queen of Peace Hospital
- New Ulm – New Ulm Medical Center
- Northfield – Northfield Hospital
- Olivia – RC Hospitals & Clinics
- Owatonna – Owatonna Hospital
- Redwood Falls – Redwood Area Hospital
- Shakopee – St. Francis Medical Center
- Sleepy Eye – Sleepy Eye Medical Center
- Springfield – Springfield Medical Center
- St. Peter – River’s Edge Hospital and Clinic
- Waconia – Ridgeview Medical Center
The Center for Aortic Disease at Allina Health Minneapolis Heart Institute – Minneapolis provides a multidisciplinary approach in caring for patients with complex aortic conditions. Our aortic program focuses on early detection, monitoring and current treatments of aortic disease.
Common Aortic disorders
- Aortic aneurysms (thoracic and abdominal)
- Aortic dissections
- Bicuspid aortic valve disease with aortopathy
- Marfan’s disease
- Connective tissue disorders such as Ehlers-Danlos Syndrome, Turner’s syndrome or aortitis
- Family history of aortic conditions
Our capabilities and treatments
- Comprehensive evaluation
- CT and MRI
- Echo
- Use of minimally invasive endovascular aortic grafts
- Repair of thoracic and abdominal aneurysms
- Thoracic endografts techniques (TEVAR)
- Fenestrated graft procedures
- Thoracoabdominal surgery
- Complex valve sparing aortic replacement procedures
- Percutaneous interventions for aortic dissections
Fenestrated stent grafts
Abbott Northwestern is the first hospital in the Twin Cities area, and one of the few centers in the United States, to offer high surgical risk patients the endovascular option of fenestrated stent grafts. Each graft is customized to fit each patient and designed using a complex 3-D analysis to obtain the perfect fit.
Since the beginning of 2014, more than 30 “high surgical risk” patients have been treated using custom-made fenestrated stent grafts with a 100 percent technical success rate. Thanks to this technique, patients who have been denied surgery in the past can be successfully treated at the Center for Aortic Disease.
Hybrid cardiovascular operating room
The first hybrid room in the Twin Cities was opened at Abbott Northwestern Hospital. The room blends the capabilities of a cardiovascular catheterization laboratory with a traditional surgical suite.
The suite, which is large enough for a dozen clinicians to work seamlessly, has the appropriate technology and space for the Center for Aortic Disease’s multidisciplinary team and also features robotic three-dimensional imaging.
Allina Health Minneapolis Heart Institute Center for Complex Coronary Interventions at Abbott Northwestern Hospital provides state-of-the-art treatment to patients with complex coronary artery disease. This includes patients with chronic total occlusions, recurrent in-stent restenosis, heart failure, calcification and tortuosity. The center features an experienced, world-class care team that has access to advanced equipment and cutting-edge techniques.
The team offers:
- Hemodynamic support
- Coronary brachytherapy
- Treatment for chronic total occlusion
Patient image transfer
Thank you for entrusting us in the ongoing care of your patient.
Chronic total occlusion
Minneapolis Heart Institute® offers cutting-edge treatment for coronary chronic total occlusion (CTO), blockages of the coronary arteries that have been present for at least three months. We offer diagnosis and treatment for CTOs, including:
- Medication
- Surgery
- Minimally-invasive procedures
Resources
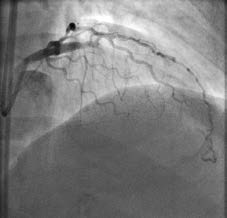
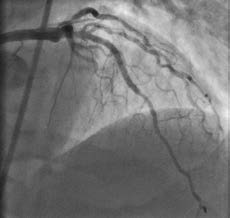
Coronary angiogram immediately following successful stenting of the occlusion using the reverse controlled antegrade and retrograde tracking (CART) technique. Allina Health Minneapolis Heart Institute was the first center in the Upper Midwest to use this novel approach to open chronic total occlusions and it now trains interventional cardiologists at other regional centers in using the technique.
Since performing the first coronary angioplasty in the Twin Cities in 1978, Allina Health Minneapolis Heart Institute at Abbott Northwestern Hospital has become a regional and nationally recognized leader in coronary therapeutics.
By participating in multiple large clinical trials and performing complex coronary interventional procedures, Minneapolis Heart Institute® has developed innovative programs to treat coronary artery disease, cardiac emergencies and structural and valvular heart disease. Interventional cardiologists are dedicated to advancing new and novel approaches to cardiovascular therapeutics.
Modeled after the world-renowned Center for Hypertrophic Cardiomyopathy, the Center for Genetic Arrhythmias focuses on the diagnosis, treatment and research related to five additional life-threatening arrhythmic conditions:
- Long QT syndrome
- Arrhythmogenic right ventricular dysplasia
- Brugada’s syndrome
- Left ventricular noncompaction
- Catecholamine-induced, polymorphic, ventricular tachycardia
The Genetic Arrhythmias staff can screen, diagnose and care for entire families who have been affected by one of these conditions. Ongoing research—including a comprehensive registry of the family medical history—examines protocols and evaluates treatment plans, giving hope to subsequent generations. We have experts in advanced cardiovascular imaging, electrophysiology, cardiology, genetic counseling and clinical nursing. Team members obtain exhaustive assessments, chart the natural history of these conditions and determine how to most efficiently and effectively care for patients and their families.
The team also works directly with the world renowned Jesse E. Edwards Registry of Cardiovascular Disease at United Hospital in St. Paul, part of Allina Health, to diagnose conditions that have resulted in sudden cardiac death. These results then can be used to screen and evaluate surviving family members. Established in 1960, the Registry has examined more than 24,000 cardiac specimens and is a vital repository of knowledge.
Allina Health Minneapolis Heart Institute at Abbott Northwestern Hospital features one of the largest and most comprehensive arrhythmia programs in the country. Our team of electrophysiologists, skilled technicians, advanced practitioners and nurses collaborate closely to provide a full range of services and personalized care for heart rhythm management. We specialize in treating patients with complex conditions and perform nearly 1,900 procedures each year.
The heart rhythm management team establishes close partnerships with referring physicians, patients and families regarding complex treatment plans. We are dedicated to educating and empowering cardiovascular professionals and those impacted by life-threatening arrhythmias.
The program offers extensive expertise and cutting-edge technology in the following areas:
Complex ablation procedures using 3D mapping systems
- Atrial fibrillation
- Epicardial ablation
- Ventricular tachycardia
- Arrhythmias associated with congenital heart disease
Lead extraction with laser assistance and surgical back-up
- Advanced ablation techniques
- Cryoballoon
- Surgery for atrial fibrillation (concomitant Maze procedures, minimally invasive procedures)
Cardiac device therapy for heart rhythm and heart failure management
- Including patients with genetic arrhythmias and complex congenital disease
Left atrial appendage occlusion device therapy
Hypertrophic cardiomyopathy (HCM) is the most common genetic heart disease, the most frequent cause of sudden cardiac death in the young (including trained athletes), and can be responsible for heart failure symptoms at any age. For more than 20 years, Barry J. Maron, MD, an international expert on HCM, directed the unique HCM Center at the Minneapolis Heart Institute Foundation (MHIF).
The HCM Center has led in patient care, research and teaching related to this complex disease. As the first of its kind, it is a model in delivering patient care that involves the diverse cardiovascular disciplines of electrophysiology, interventional cardiology, echocardiography and cardiovascular magnetic resonance imaging, heart failure and transplant cardiology and surgery, genetic testing and family counseling provided through strong clinical nursing. The large HCM Center cohort includes 1,500 patients from all 50 states and 25 foreign countries whose ages range from 2 to 95 years.
The Center operates on the principle that all potential complications of HCM can be effectively treated, providing the opportunity for normal life expectancy. This focused approach has substantially improved patient outcomes. Targeted strategies include using the implantable defibrillator (ICD) to prevent sudden death (the first systematic program of its kind) and surgical myectomy (in collaboration with the Mayo Clinic) to reverse heart failure, enhancing quality of life and the opportunity for normal longevity. By virtue of MHIF’s sudden death prevention initiative, 250 young patients have received life-saving ICD therapy and survive to the present.
The HCM Center, in collaboration with Allina Health Minneapolis Heart Institute’s Center for Cardiovascular Imaging, has made major advances in noninvasive diagnosis of this disease, including identifying high-risk patients with HCM whose disease might otherwise be undetected. Clinical research is a major impetus of the HCM Center, which has contributed 525 papers to the literature over 20 years that describe the diagnosis, natural history and treatment-related outcomes of patients with this complex genetic disease. This systematic series of investigations has measurably changed perceptions, management, decision-making and outcome of HCM.
Preventing heart disease or restoring your health after a heart attack or cardiac event is the goal of our preventive cardiology clinic. Heart disease continues to be the leading cause of death for both men and women. Our team of experts is committed to reducing the incidence of cardiovascular heart disease through best-practice clinical care for our patients and investigative research.
Our clinic fosters lifestyle changes and provides tailored medical treatment to:
- Manage risk factors and prevent heart disease
- Reduce the progression of heart disease for those who have had a heart attack or stroke
- Offer options for those who experience statin intolerance
- Treat familial hypercholesterolemia, a genetic disorder of LDL cholesterol
- Improve the quality of life by reducing symptoms
Know your risk
The first step in heart disease prevention is knowing your risk. Even one condition or habit makes you more likely to develop heart disease. But having more than one risk factor increases the possibility for heart disease.
- Age
- Family history of early heart disease
- Diabetes or pre-diabetes
- High blood pressure
- High cholesterol
- Tobacco use
- Lack of regular exercise
- High levels of stress
Preventive cardiology services
- A comprehensive cardiovascular examination and evaluation of cardiac risk factors
- Advanced blood tests with results at appointment
- Lipid management including statin intolerance
- Nutrition assessment and recommendations
- Cardiac Imaging (HeartScan) – access to a special scan that can detect deposits in the heart arteries before symptoms are present.
- Opportunity for participation in clinical trials of new therapies
Know Your Team
The Preventive Cardiology program is staffed by a multidisciplinary team of cardiologists, advanced care providers (nurse practitioners, physician assistant), dietitian/nutritionist, and research nurses dedicated to disease management.
Schedule an Appointment
Call 612-863-3900612-863-3900
Preventive cardiology clinics are available at:
- Abbott-Northwestern Hospital – Minneapolis Heart Institute Outpatient clinic, Minneapolis
- Allina West Health, Plymouth
- Centennial Lakes Office Building , Edina
- Chaska 212 Medical Office Building, Chaska
Allina Health Minneapolis Heart Institute is proud to offer Teleheart services in these communities across Minnesota: Blue Earth, Fairmont, New Ulm, Faribault, Olivia, Glencoe, Morris, Sleepy Eye, Pine City, Baxter, Brainerd and Crosby. We have also expanded to offer Teleheart in Fargo, ND and Naples, FL.
TeleHeart offers patients several advantages over traditional specialty care
- Shorter wait for specialty care- It offers patients faster access to Minneapolis Heart Institute® specialists, reducing the wait time for a specialty appointment.
- Convenience – Patients can receive nationally-recognized cardiovascular care without long distance travel at their community clinic. The patient’s family and support system also benefit from local care delivery instead of traveling to the Twin Cities for the initial consult and first-step diagnostic testing, which typically can be performed at an outpatient center.
- Cost to patient – The costs for TeleHealth visits are similar to traditional office visits and usually covered by medical insurance.
How it works
For a TeleHeart appointment, local nurses start the face-to-face patient visits, review patient’s presenting needs. They then connect with our cardiovascular provider with the patient via TeleHealth video equipment.
Patients can ask questions and interact, just as they would in a traditional clinic appointment. Each patient’s medical history and test results are available to the cardiovascular provider in advance of the appointment. The patient documentation appears in electronic health record in a letter format and mailed to the primary care provider. Each appointment is billable as a clinic visit. Technology used in these TeleHeart appointment may include an Internet enabled stethoscope and TeleHealth video equipment.
For more information about our TeleHeart services, sites and providers, visit allinahealth.org/teleheart.
The Center for Valve and Structural Heart Disease at Allina Health Minneapolis Heart Institute – Minneapolis is world renowned for clinical and innovative expertise. The full spectrum of state-of-the-art diagnostic testing is available. A multidisciplinary approach enables the delivery of the most innovative transcatheter and surgical therapies for treating valve and structural heart disease, including investigational approaches that are provided at only a few centers in the world.
The Center serves as a training site for multiple transcatheter and surgical therapies, and regularly teaches these approaches through live case demonstrations and high-quality didactics. In partnership with the Minneapolis Heart Institute Foundation, patients can participate in major clinical trials of valvular and structural heart disease. Current and prior studies include: Tendyne transcatheter mitral valve replacement Global Early Feasibility Study, Medtronic Intrepid transcatheter mitral valve replacement Global Early Feasibility Study, PARTNER 1, PARTNER 2, S3i CAP, SURTAVI, COAPT, REPRISE III, REPRISE III CAP, Myocor, PORTICO, EVEREST, and REALISM. A selected bibliography with highlights of this research is shown below.
In April 2015, the first transcatheter mitral valve replacement in the U.S. was performed at Allina Health Minneapolis Heart Institute and it continues to have the highest volume, in the world, of patients for this novel procedure.
Clinical practice
Our physicians, surgeons, and care providers see patients in a dedicated clinic, where a multidisciplinary, heart-team approach is highly valued. These subspecialists also participate in a weekly conference, where patient care is reviewed and discussed for consensus in diagnostic and treatment plans, and for coordination of services.
State-of-the-art therapies available (selected list):
- Transcatheter mitral valve repair (MitraClip)
- Transcatheter mitral valve replacement for native mitral regurgitation
- Valve-in-valve therapy for prosthetic valve degeneration
- Minimally-invasive mitral valve surgery (e.g., port access)
- Mini-sternotomy aortic valve surgery
- Paravalvular prosthetic leak repair
- Transcatheter tricuspid valve repair
- Balloon mitral valvuloplasty
- Balloon aortic valvuloplasty
- Alcohol septal ablation
- Ventricular and aortic pseudoaneurysm transcatheter repair
- Transcatheter closure of patent foramen ovale (PFO), atrial septal defect, and ventricular septal defect
Presentations on valvular heart disease
Patient image transfer
Thank you for entrusting us in the ongoing care of your patient.
Our valve subspecialists in interventional cardiology, cardiac surgery and advanced cardiovascular imaging work as an integrated team to offer the full spectrum of traditional and pioneering valve therapies. The valve team meets weekly to discuss complex and high-risk patients and determine the most appropriate therapy, including options for leading-edge interventions.
Valve subspecialists and valve nurse coordinators are available to answer referring physicians’ questions regarding traditional valve therapies as well as patient eligibility for investigational percutaneous trials. Allina Health Minneapolis Heart Institute – Minneapolis is a regional valve center of excellence with a hybrid operating room designed for transcatheter and minimally invasive surgical valve procedures. These high tech rooms have the advanced imaging systems necessary for repairing and implanting valves often through very small incisions necessitating indirect visualization.
Patient image transfer
Thank you for entrusting us in the ongoing care of your patient.
Transcatheter Treatments for Valvular Heart Disease
Aortic balloon valvuloplasty is a percutaneous procedure for symptom palliation and enhanced quality of life in appropriately selected patients who are not candidates for surgical or transcatheter aortic valve replacement. Further, it can be a useful bridge for select patients to undergo subsequent surgical or percutaneous aortic valve replacement. Allina Health Minneapolis Heart Institute is a recognized world leader in establishing and performing this therapy and is one of the highest volume centers in the country.
The team also has extensive experience in mitral and pulmonic balloon valvuloplasty, which unlike aortic valvuloplasty, are treatments of first choice for mitral and pulmonic stenosis. Allina Health Minneapolis Heart Institute Aortic Balloon Valvuloplasty Database has shown that among patients who have had the procedure:
- More than 90 percent achieve >30 percent improvement in aortic valve area
- More than 90 percent achieve New York Heart Association functional class of ≤ 2 with sustained benefit for 0.5-1.5 years
- Less than 3 percent experience complications
Valve Center physicians’ published studies have shown that the procedure can be safely performed:
- In patients over 90 years of age
- In combination with coronary stenting
- In patients with severe left ventricular dysfunction (including LVEF <20>
Transcatheter aortic valve replacement (TAVR) is a revolutionary percutaneous therapy for aortic valve replacement. At present, however, this therapy can be offered only to patients who are nonoperative or high risk for traditional open heart surgery. The Valve Center currently performs TAVR using transfemoral or transapical approaches, both of which are now approved by the Food and Drug Administration (FDA).
Transcatheter (percutaneous) mitral valve repair is an investigational option for the treatment of high surgical risk patients with severe mitral regurgitation. The Valve Center is currently evaluating the MitraClip system in these patients. Watch this video to learn more about the latest advances in treating heart failure or leaky valves with MitraClip.
Percutaneous repair of periprosthetic valve leaks addresses perivalvular leaks that can be severe in 1 to 2 percent of patients following surgical valve replacement. This option avoids the need for a second open heart surgery, but it is a technically demanding procedure performed at only a few centers in the U.S.
Surgical Replacement and Repair
Allina Health Minneapolis Heart Institute‘s cardiac surgeons offer surgical valve replacement and repair using conventional and minimally invasive approaches to best meet patients’ needs. Surgical replacement or repair is the recognized gold standard for treatment of valvular disease.
Treatments for Other Structural Diseases
The atrial septal defect (ASD)-patent foramen ovale (PFO) percutaneous closure program is well established. Since 2003, Allina Health Minneapolis Heart Institute has done more than 300 procedures with a minimal complication rate. Careful patient selection, advanced CT and TEE imaging, including 3D TEE and intra-cardiac echo, help make this possible. Newer guidelines, based on recent clinical trials, and American Heart Association and American College of Cardiology position statements currently favor a more conservative approach in patients with PFO and stroke. Our physicians incorporate these newer guidelines into their practice, which is tailored to each individual patient to provide the best possible care.
At this nationally recognized center, specialists from vascular surgery, endovascular surgery, interventional radiology, advanced cardiovascular imaging, vascular medicine and vascular nursing collaborate to provide the most advanced care for patients with vascular disease.
Patients benefit from the Center’s comprehensive diagnostic and treatment services provided by specialists dedicated to the field of vascular disease. They may also have the opportunity to enroll in regional and national multi-center clinical trials that offer new therapies and treatment options. Vascular and endovascular services are designed to diagnose and prevent disease progression, provide ongoing therapy, preserve independence and improve quality of life.
- Abdominal aortic aneurysm
- Complex aortic pathology
- Thoracic/thoracoabdominal aneurysm
- Aortic dissection (acute and chronic)
Carotid and Vertebral Artery Disease
- Carotid endarterectomy
- Carotid angioplasty/stenting
- Vertebral artery reconstruction
Peripheral Artery Disease (PAD)
- Claudication
- Critical limb ischemia
Advanced Peripheral Arterial Disease (APAD) Center
- Comprehensive CV imaging
- Advanced non-invasive studies
- Minimally-invasive interventions to treat arterial disease
- Emergency care for critical limb ischemia
- Wound care clinic
- Hyperbaric Oxygen Therapy
- Access to clinical trials for the latest medial and interventional therapies
Renal Artery and Mesenteric Arterial Disease
- Refractory hypertension
- Mesenteric ischemia
Venous Disease
- Varicose veins and venous insufficiency
- Non-invasive evaluation
- Radiofrequency ablation
- Sclerotherapy
- ClariVein®
- VenaSeal™
Advanced Endovascular Procedures
Patients have access to the most advanced, minimally invasive treatments, including:
- Endovascular abdominal aortic aneurysm repair
- Endovascular thoracic aneurysm repair
- Percutaneous revascularization of lower extremity PAD
- Renal/mesenteric stenting
- Carotid stenting
- Stent-graft therapies for complex aortic pathology
Vascular Medicine
Vascular medicine services involve preventing, diagnosing and managing arterial, venous and lymphatic disorders. Diagnostic services include physiologic and radiologic lab testing and test interpretation. Conditions treated include:
Arterial Disease
- Vasoactive disorders: Raynaud’s, acrocyanosis, erythromelalgia, frost bite and pernio chilblains
- Vascular compression: thoracic outlet, median arcuate ligament and nutcracker syndromes, popliteal entrapment and external iliac artery endofibrosis
- Vasculitis: large, medium and small vessels
Venous Disease
- Varicose vein and venous insufficiency using chemical and endothermal ablation
- Deep vein thrombosis and pulmonary embolism
- Management of Bleeding Associated with the Novel oral Anticoagulants
- Thrombophilia and hypercoagulation testing, anticoagulation management and using new anticoagulation agents
- Anticoagulation before and after procedures
- Lymphatic disease
- Congenital and secondary lymphedema
Congenital Syndromes
- Fibromuscular dysplasia, vascular malformation, segmental arterial mediolysis, Klippel-Trenaunay Syndrome, May Thurner Syndrome, Von Hippel Lindau disease, and connective tissue disorders including Marfan and Ehlers-Danlos syndromes.
Wound Clinic and Hyperbaric Oxygen Therapy Program
Abbott Northwestern Hospital’s multidisciplinary Wound Clinic is staffed by vascular surgeons, vascular medicine physicians, general surgeons, plastic surgeons, infectious disease specialists, podiatrists, advanced practice providers and nurses specializing in wound care. The Wound Clinic provides a variety of treatment options to promote wound healing, including hyperbaric oxygen therapy, which stimulates angiogenesis by delivering 100 percent oxygen at elevated barometric pressure.